Edit Claim - Medical Tab
Enter necessary information when billing to medical insurance in the Medical tab of a claim.
In a Claim, click the Medical tab.
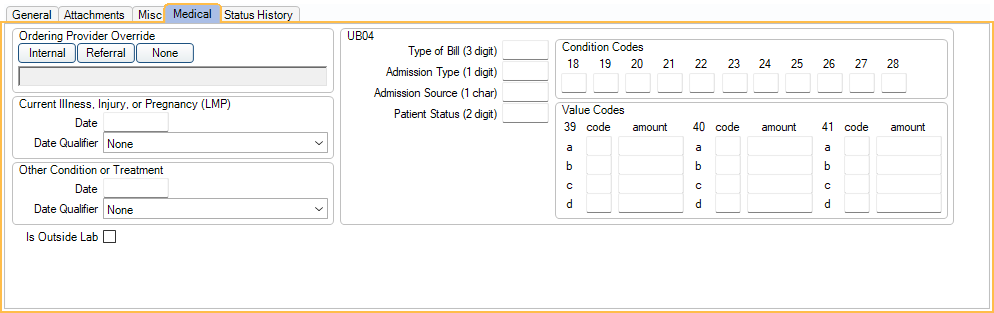
Only visible if Medical Insurance is turned on. Only enter information on this tab when sending a medical claim.
Ordering Provider Override: Set a general ordering provider override for procedures on this claim. This override is only assigned to procedures on the claim that do not have an override set on the procedure level (Procedure - Medical Tab). By default, there is no override and the treating provider is used. See E-Claims Complexities, Ordering Provider, for the logic.
- Internal: Select a provider from the Providers list.
- Referral: Select a provider from the Referral List.
- None: Clear the override.
UB04: The UB04 is typically used for institutional claims (e.g., hospitals or outpatient facilities). The Claim Forms are printed; they are not sent in e-claims. Check with the insurance company to verify the values they accept for items in this section.
Information on codes used on a UB04 claim cannot be published by Open Dental and is owned by the American Hospital Association.
Printing: It is helpful to have a background image for setup purposes. The background image should not be set to print as preprinted forms should be used. To see the background, save the file UB04.jpg in the A to Z Folder (i.e., OpenDentImages folder), then add it to the Claim Form.

